There has been a steady stream of headlines declaring that life expectancy in the United States is decreasing.
And the often-cited reason is the climbing number of opioid-related deaths.
Those two facts piqued the interest of a group of researchers who sought to reframe the way these trends can be viewed.
“We have a problem that is otherwise being underestimated,” said Ian Rockett, an injury epidemiologist and professor emeritus at West Virginia University.
Suicide rates have been steadily climbing, Rockett said, but their numbers are likely even higher. He said too often opioid-related drug overdoses aren’t classified as suicides, and he thinks they should be.
These deaths are often deemed by medical examiners as “accidental injury deaths” unless a suicide note is found. This classification doesn’t take into account that suicide and drug overdoses both arise from “purposeful” behaviors.
To get at the root of that problem, Rockett and his colleagues developed a model of self-injury mortality that factors together both categories — overdose deaths and suicides. This combined classification “is intended to promote prevention and earlier interventions” by recognizing common, preexisting mental health issues that could have been in play, the researchers wrote.
“By always separating drug deaths from suicide is to underestimate the mental health crisis,” Rockett said. “These are all mental health issues, and they need to be on the front burner.”
The report, published Monday in the British journal Injury Prevention, shows that together these deaths would become the seventh leading cause of death in the U.S., just surpassing diabetes.
It also focuses attention from lawmakers and health practitioners on the nation’s mental health crisis and how both suicide and overdose death rates highlight the system’s gaps. Rockett conducted a similar study two years earlier.
“When a death is an accident, there’s a tendency for people to say, ‘Nothing we could do about that.’ By putting the emphasis on self-injury, we draw greater attention to the problem and particularly as an overriding mental health issue,” Rockett said.
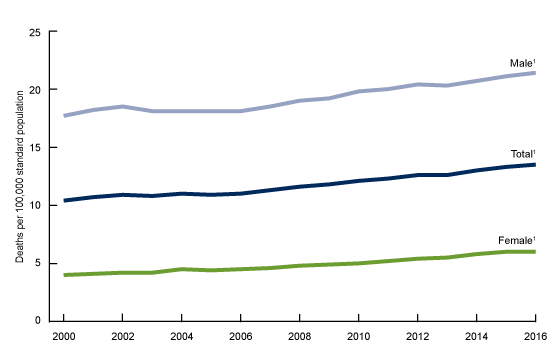
According to CDC data, the incidence of suicide increased from 10.4 deaths per 100,000 in 2000 to 13.5 per 100,000 in 2016.
Rates of drug overdose deaths have increased threefold, from 6.1 out of 100,000 deaths in 1999 to 19.8 deaths per 100,000 in 2016.
Rockett found that in 2016, the most recent year for which data is available, self-injury deaths accounted for 29.1 out of every 100,000 deaths.
But not everyone is sold on Rockett’s concept.
“I understand what he’s trying to do, I’m still not sure of the utility of combining these,” said Bob Anderson, the chief of the mortality statistics branch at the National Center for Health Statistics at the Centers for Disease Control and Prevention.
There’s overlap between drug overdose deaths and suicides, Anderson said, adding that suicides by overdose are underestimated in general.
“I don’t dispute [Rockett’s] conclusions,” he said, although he suggested not all overdoses should be considered the same as suicides.
“By lumping all of them into one category we may miss some important distinctions that need to be made,” he added.
Kaiser Health News, a nonprofit health newsroom whose stories appear in news outlets nationwide, is an editorially independent part of the Kaiser Family Foundation.


