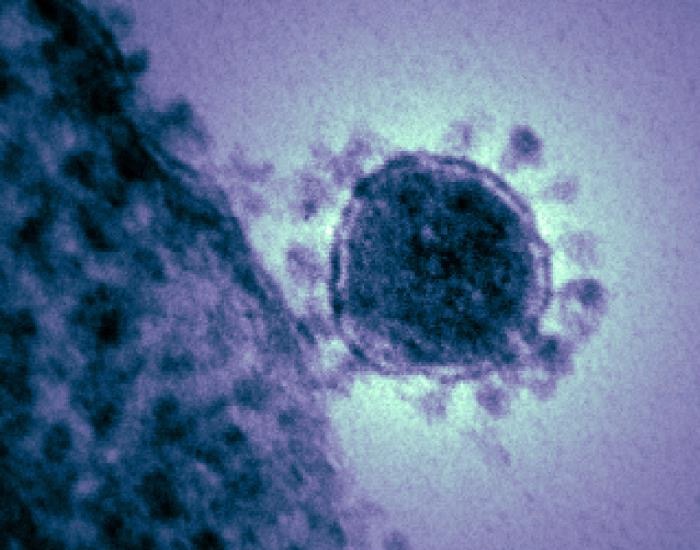
The 2019 novel coronavirus outbreak and pandemic preparedness
As the 2019 novel coronavirus outbreak continues to expand in China, and the World Health Organization has now declared a global public health emergency, it raises questions about what it means for the United States and locally here in King County.
While there is not currently sustained transmission of the virus in the US, the situation continues to evolve rapidly, and local public health officials continue to be vigilant.
To help understand what this could mean for us, and how we can be prepared as a community, we sat down with Dr. Jeff Duchin, Health Officer for Public Health – Seattle & King County to learn more.
What’s the difference between an outbreak, an epidemic and a pandemic?
An epidemic (or outbreak) refers to an increase, often sudden, in the number of cases of a disease above what is normally expected in that population in that area. A pandemic is the worldwide spread of a new disease, usually affecting many people.
What are some examples of pandemics?
Recent spread of diseases like SARS, Ebola, and Zika demonstrate that emerging outbreaks are the new normal, and illustrating that a disease outbreak anywhere can lead to a disease outbreak everywhere.
Not all emerging diseases become pandemics, however. In recent times, most pandemics have been due to newly emerging influenza viruses: the Spanish flu (H1N1) in 1918-1920, the Asian flu (H2N2) in 1957-1958, the Hong Kong flu in 1968-1969, and most recently the Avian flu (H1N1) 2009. In 2016, the Zika virus emerged and spread causing a global pandemic.
Are all pandemics the same in terms of severity?
Pandemics are defined by their wide spread across the globe, but their severity can depend on many interrelated factors, including characteristics of the infection itself: the severity of illness; the route and rapidity of spread; the underlying health and susceptibility of the population and subgroups within the population; and prior history of population exposure to similar infections.
It also depends on the strength of health systems to respond, including the general healthcare system quality and accessibility; availability of treatment and preventive measures; and the capacity and capability of national, state and local public health and clinical health care and emergency response systems.
There are other important factors at play as well, including the quality and availability of timely and accurate communication; the level of trust in public health, medical and local governmental authorities; and community-level preparedness and resilience across many sectors, including business, government, schools, critical infrastructure, and other services.
Are we prepared for a pandemic?
A recent report found that the United States is the most prepared country in the world to respond to an emerging pandemic. The 2019 Global Health Security Index, a comprehensive assessment and benchmarking of health security and related capabilities, ranked the US most prepared out of 195 countries evaluated.
In addition, Washington state is rated among the most prepared states in the US for public health emergency response.
That said, relative preparedness does not mean perfectly prepared for any and all unforeseen challenges, and there are real opportunities for improvement. Pandemic preparedness requires sustained funding and commitment of resources.
Washington state is rated among the most prepared states in the US for public health emergency response.
Dr. Jeff Duchin – Public Health – Seattle & King County
Current gaps in our preparedness include the need for more rapid development and availability of point-of-care diagnostic tools, medical treatments and vaccines, and maintaining a robust public health and healthcare system baseline response and emergency surge capacity.
It’s critical for our federal government to renew our national commitment to health security, public health, health care system and community level preparedness.
How would a serious pandemic challenge us?
We should assume that a large-scale health emergency like a serious pandemic will, for some limited but undefined time period, stress our healthcare, public health and other community support systems, and pose communication challenges requiring clear and accurate messages from authoritative sources and constant vigilance for misinformation. An event like this has the potential to significantly disrupt business as usual across many sectors of the community with corresponding economic impacts.
How does a new infection spread in a community?
It’s primarily about how people interact. The ease with which a disease spreads in a community is related to the intensity, type and duration of interpersonal interactions across various age groups.
How readily an infection spreads in a population is influenced by factors like the frequency, nature and intensity of person-to-person contacts; mixing patterns in family, work, social, and school settings, human behaviors, and the use of personal protective measures (like hand and respiratory hygiene and staying home when sick), the age distribution of the population, environmental factors, and even the season of the year. These factors can differ between countries and communities and influence how effectively a disease spreads in one place or time compared to another.
Can you say more about the importance of good communication in health emergencies?
Unfortunately, we know that in newly emerging outbreaks some people will spread inaccurate information, incite fear, and promote discrimination leading to stigmatization of others because of their appearance, race or ethnicity.
It’s important to counter inflammatory and false messages with accurate, evidence-based information. We cannot let the first casualties of the novel coronavirus infection be good judgement, rational thought and respect for all of our community members regardless of their ancestry.
What is the status of the current 2019 novel coronavirus (2019 nCoV) outbreak?
At this time, much remains unknown about the true severity and transmission characteristics of the 2019 novel coronavirus, and we can’t predict what the ultimate course of this outbreak will be or if it becomes a global pandemic, how severe it might be in the US.
Early on during newly emerging infectious disease outbreaks, the severe cases that are hospitalized and the deaths are identified and reported while milder and possibly asymptomatic cases are not recognized. If there are many less serious illnesses that are not counted, the severity appears much higher than it actually is.
When new infections are emerging, we expect uncertainty about key issues that decreases over time as we learn more. Our public health, medical and community response strategies will evolve to reflect new information as it becomes available. Ultimately, if this disease becomes established in the human population, the development of treatments and vaccines may help prevent ongoing risk, much like we use for influenza.
Does the fact that the World Health Organization (WHO) declared the 2019 nCoV outbreak to be a global public health emergency change anything here locally?
Absolutely not. Since the first case of novel coronavirus infection in a Snohomish County resident was announced on January 21st our public health system has been firing on all cylinders to do all we can to identify local cases of and prevent spread to others.
The WHO announcement is important to mobilize a coordinated international response to the outbreak in China and other countries but does not impact local preparedness and response efforts in any way.
What’s the bottom line for now?
The bottom line is that currently, the risk of novel coronavirus infection to the public in the US remains low, although that may change. There are few cases in the US and the cases have been promptly identified and isolated. For perspective, it’s useful to remember that each year in the US, between 9 – 45 million people are infected with influenza resulting in 12,000 to 61,000 deaths, despite widespread availability of antiviral treatment and effective vaccines.
Even though we cannot predict the course of the 2019 novel coronavirus outbreak, it presents a good opportunity for all of us, in public health, government, healthcare, business, and community organizations alike to review their emergency and pandemic response plans. Whether it be novel coronavirus, an earthquake or the next inevitable emerging infectious disease, we know that preparedness planning pays off.
You can find current accurate information on the evolving outbreak from CDC at https://www.cdc.gov/coronavirus/2019-nCoV/index.html and Public Health – Seattle & King County at www.kingcounty.gov/ncov.


