Category: Vaccines
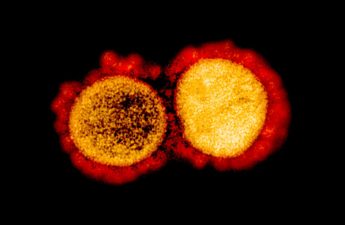
Study confirms link between COVID-19 vaccination and temporary increase in menstrual cycle length
On average, vaccinated people experienced an increase of less than one day in each cycle in which they were vaccinated: a .71 day increase after the first dose and a .56 day increase after the second dose. Participants who received both doses in a single cycle had a 3.91 day increase in cycle length.
Most States Are Wary of Mandating COVID Shots for Kids
Many parents who have not gotten their children vaccinated say the absence of full FDA authorization is a factor, since it suggests that the vaccines have not been fully vetted.
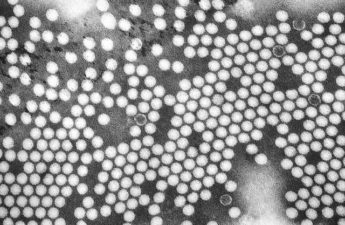
Fears of a polio resurgence in the US have health officials on high alert
A virologist explains the history of this dreaded disease
Omicron COVID-19 vaccine boosters now authorized for certain individuals
New boosters aim to provide better protection from currently-circulating variants of COVID-19
When can I get the updated covid booster — Public Health – Seattle & King County
The very earliest we could expect to have the new booster doses available at our vaccination sites at the Auburn Outlet Collection Mall would be the weekend of September 9th. However, delays in shipping are possible, so it could be later.
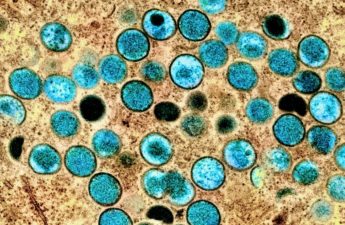
Monkeypox in King County: An Update
As of today, 310 King County residents have been diagnosed with MPV, an increase from 48 cases in mid-July.
How does monkeypox spread?
The current monkeypox epidemic is a bit unusual in a few ways: First, the sheer scope of the current epidemic; Second, the way symptoms are appearing may facilitate spread among people who don’t yet know they are infected.
How Misinformation About COVID Vaccines and Pregnancy Took Root Early On and Why It Won’t Go Away
Before coronavirus vaccines were even released, a disinformation campaign used a moment of national and personal vulnerability to prey on those who were pregnant or who planned to become pregnant.
Monkeypox: an expert explains what gay and bisexual men need to know
While anyone can get monkeypox, the current outbreak is overwhelmingly affecting sexually active gay, bisexual and other men who have sex with men.
NY polio case linked to overseas virus
Rockland County, a suburban area northwest of New York City, sought medical treatment in June for weakness and paralysis. He had not been vaccinated against polio.
Monkeypox Straining Already Overstretched Public Health System
Echoing the early days of the COVID-19 pandemic, demand for monkeypox vaccine doses far outstrips supply, appointments have been difficult to get, and money and personnel have had to shift from other priorities.
Boost Now or Wait? Many Wonder How Best to Ride Out Covid’s Next Wave
Consistent messaging has been complicated by the different views of leading vaccine scientists. Although physicians like del Rio and Dr. Peter Hotez of Baylor College of Medicine see the value in getting a second booster, Dr. Paul Offit, a member of the FDA’s vaccine advisory committee, is skeptical it’s needed by anyone but seniors and people who are immunocompromised.
Monkeypox FAQ:
How is it transmitted? Where did it come from? What are the symptoms? Does smallpox vaccine prevent it?
Should you get a COVID-19 booster shot now or wait until fall? Two immunologists help weigh the options
Clinical studies show that mixing and matching booster vaccines can lead to a more robust immune response.
Will the US Overcome Its Covid Complacency Even as the Threat Returns?
Two years ago, pre-vaccine, the images of dying people on ventilators saying goodbye on iPads, doctors in hazmat suits, and portable morgues in hospital parking lots briefly engaged everyone in the need for public health resources, and Congress stepped up. Now, the public has moved on. But the threat hasn’t gone away. And there will be a price to pay.