Category: Pregnancy
Prenatal supplements fall woefully short in providing crucial nutrition during pregnancy – and most women don’t even know it
Prenatal supplements are not the insurance plan that many doctors believe them to be.
The number of births continues to fall, despite abortion bans
Births continued a historic slide in all but two states last year, making it clear that a brief post-pandemic uptick in the nation’s birth numbers was all about planned pregnancies that had been delayed temporarily by COVID-19.
The Powerful Constraints on Medical Care in Catholic Hospitals Across America
More than half a million babies are born each year in the U.S. in Catholic-run hospitals, including those owned by CommonSpirit Health, Ascension, Trinity Health, and Providence St. Joseph Health. That’s 16% of all hospital births each year, with rates in 10 states exceeding 30%. In Washington, half of all babies are born at such hospitals, the highest share in the country.
Telehealth makes timely abortions possible for many, research shows
Access to telehealth abortion care can determine whether a person can obtain an abortion in the United States. For young people and those living on low incomes, telehealth makes a critical difference in getting timely abortion care.
There’s a new pill for postpartum depression, but many at-risk women face hurdles
Suicide and overdoses are among the leading causes of maternal death in the U.S.
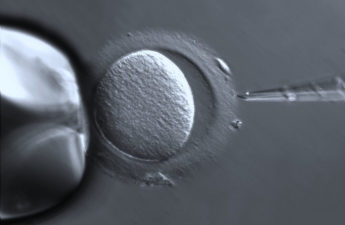
Viewpoint: Restricting Obese Women From IVF Is Discriminatory
Fertility clinics bar women with obesity from their services, despite the lack of medical evidence for doing so.
US birth rates are at record lows – even though the number of kids most Americans say they want has held steady
Birth rates are falling in the U.S. Is this decline because, as some suggest, young people aren’t interested in having children? Or are people facing increasing barriers to becoming parents?
Medical exceptions to abortion bans often exclude mental health conditions
Despite mental health conditions making up more than 20% of maternal deaths and 1 in 5 women suffering maternal mental health conditions, several states explicitly exclude mental health conditions as exceptions to abortion restrictions.
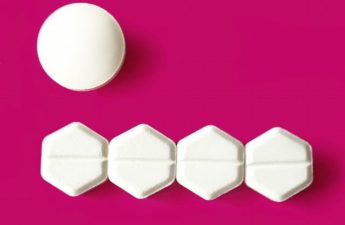
Many women can’t access miscarriage drug because it’s also used for abortions
Doctors say patients have gotten caught up in larger debates around abortion
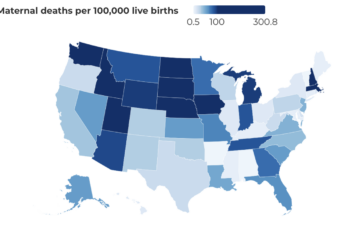
Risk of death related to pregnancy and childbirth more than doubled between 1999 and 2019 in the US, UW study finds
Most maternal deaths are considered preventable because, in the U.S., maternal deaths are most often caused by problems that have very effective treatments, including bleeding after delivery, heart disease, high blood pressure, blood clots and infections.
COVID-19 vaccination and boosting during pregnancy benefits pregnant people and newborns
The researchers found that pregnant women who received the COVID-19 vaccines generated antibodies against specific types of SARS-CoV-2. These antibodies crossed the placenta and were also found in the cord blood of vaccinated participants. This likely conferred some protection in the newborns against infection immediately after birth—a critical time when they are vulnerable to severe COVID-19 disease but are too young to be vaccinated.
Vaccination in pregnancy greatly reduces risk of severe illness and death from COVID-19, and protects babies up to 6 months after birth
Extensive evidence shows COVID-19 vaccinations in pregnancy are safe, when given at any time during the pregnancy.
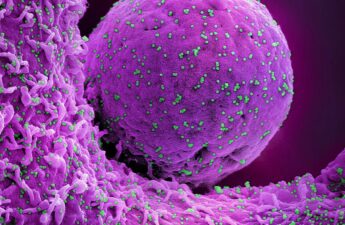
Cytomegalovirus lies dormant in most US adults and is the leading infectious cause of birth defects, but few have heard of it
“Why didn’t anyone tell me about this virus?” is a frequent response I hear from parents upon learning their newborn is infected with cytomegalovirus, or CMV. Although more than half of the U.S. population will be infected with CMV by the age of 40 and the disease is common worldwide, few people have ever heard of it.
Anti-mifepristone court decisions rely on medical misinformation about abortion and questionable legal reasoning
All the risks associated with medical abortion – and therefore the time and resources doctors must spend caring for patients – will be higher if pregnant people are compelled to have surgical abortions or to give birth.
Planning for a baby? Why both men and women should consider quitting alcohol before and during pregnancy
While the focus tends to be on a woman’s use of alcohol before and during pregnancy, an increasing amount of evidence indicates that men’s alcohol use also plays a role when it comes to the health of the baby. Indeed, alcohol can affect sperm DNA, in some cases reducing fertility and the potential to conceive.