Category: Breast Cancer
How to assess your risk for breast cancer
One in eight American women will develop breast cancer in their lifetime. A combination of factors can influence your risk.
Some are unmodifiable, such as age, having dense breasts and a family history of breast or ovarian cancer, while others are modifiable, such as physical activity levels, weight and reproductive history.
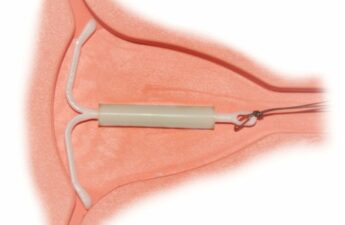
Do IUDs cause breast cancer? Here’s what the evidence says
For every 10,000 women, this study suggests we might see an extra 14 cases of breast cancer after up to five years of use, 29 cases after 5–10 years use, and 71 cases after 10–15 years use. In “absolute” terms – as a proportion of all the IUD users – all of these risk increases are comfortably under 1%.
Health News Headlines
Hospital sued over abortion denial – Breast cancer on rise among young women – Hidden liver disease – Obesity first health care – Marburg in Rwanda
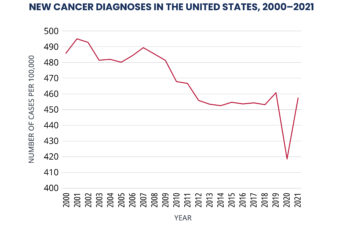
New cancer diagnoses did not rebound as expected following pandemic
Cancer incidence trends in 2021 largely returned to what they were before the COVID-19 pandemic, according to a study by researchers at the National Institutes of Health (NIH).
However, there was little evidence of a rebound in incidence that would account for the decline in diagnoses in 2020, when screening and other medical care was disrupted.
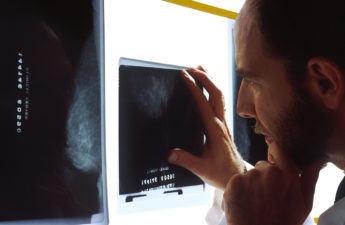
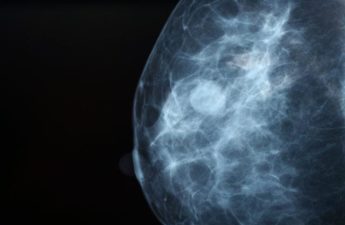
Breast density and mammograms: New FDA rule will ensure all women have more information after cancer screenings
Standard mammograms use X-rays to produce two-dimensional images of the breast. A newer type of mammography imaging called tomosynthesis produces 3D images, which find more cancers among women with dense breasts. So, researchers and doctors generally agree that women with dense breasts should undergo tomosynthesis screening when available.
Elle Macpherson’s breast cancer: when the media reports on celebrity cancer, are we really getting the whole story?
Media coverage of Macpherson’s situation has largely missed a key piece of information: her breast cancer is not invasive.
‘I’m not going to be cured’. How breast cancer awareness and support sidelines people with metastatic disease
There have been incredible advances in breast cancer diagnosis and treatment in recent years. And stories about celebrities who have “beaten” breast cancer continue to be a source of inspiration for many people. However, this emphasis on fighting, beating and surviving cancer shuts out the voices of those who will not survive. That is, the many people diagnosed with incurable, life-limiting metastatic breast cancer.
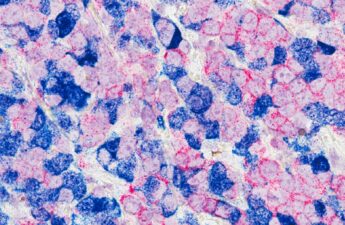
What to Know About Metastatic Breast Cancer
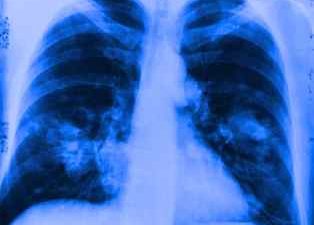
When cancer cells break away from a tumor, they can travel to other parts of the body. Metastatic breast cancer happens when cancer that began in the breast spreads (metastasizes) to other parts of the body, such as nearby lymph nodes, bones, liver, and lungs. It is also different than other stages of breast cancer, as it means you will likely have breast cancer for the rest of your life.
Study Adds to Debate about Mammography in Older Women
Studies have shown that routine screening mammography does reduce breast cancer deaths in women aged 40 to 75. But screening also comes with downsides, which include the risk of overdiagnosis and overtreatment. A new study suggests that the risk of overdiagnosis with routine screening mammography is substantial for women in their 70s and older.
Women treated for breast cancer may age faster than cancer-free women
Among women diagnosed with breast cancer, the association with faster biological aging was most pronounced for those who received radiation therapy, while surgery showed no association with biological aging.
The FDA’s rule change requiring providers to inform women about breast density could lead to a flurry of questions
Breast density matters for two reasons. Most importantly, dense breast tissue can hide cancer on a mammogram. About 40% of breast cancers will go unseen on mammography in the densest breasts, labeled “extremely dense breasts,” and about 25% will go undetected in heterogeneously dense breasts.
Breast cancer: progestogen-only and combined birth control both increase risk – here’s what you need to know
Until now, it was thought that only the combined hormonal pill carried a greater risk of breast cancer. But a recent study suggests that the progestogen-only pill (also known as the mini pill) and other forms of hormonal contraception also carry the same increase in breast cancer risk as the combined pill.
After breast cancer: 5 changes you can make to stay healthy
So, what can you do to improve your chances of living a longer, healthier life after a breast cancer diagnosis?
Cancer death rates fall among Black Americans but remain higher than other groups
Black men and women had higher rates of cancer death, both overall and for most cancer types, than White, Asian or Pacific Islander, American Indian/Alaska Native, and Hispanic/Latino men and women.
Gene Screenings Hold Disease Clues, but Unexplained Anomalies Often Raise Fears
Many genetic findings are ambiguous, leaving doctors uncertain about whether a particular variant is truly dangerous.