Category: Emergency Medicine
Out-of-hospital cardiac arrests in King County spiked during pandemic, UW study finds
Out-of-hospital cardiac arrests rose by 19% and survival of those events fell by about 4% during the first two years of the COVID-19 pandemic. But acute infections of the SARS-CoV-2 virus appeared not to be a primary cause of the changes.
Doctors Are Disappearing From Emergency Rooms as Hospitals Look to Cut Costs
This staffing strategy has permeated hospitals, and particularly emergency rooms, that seek to reduce their top expense: physician labor. While diagnosing and treating patients was once their domain, doctors are increasingly being replaced by nurse practitioners and physician assistants, collectively known as “midlevel practitioners,” who can perform many of the same duties and generate much of the same revenue for less than half of the pay.
States Strive to Reverse Shortage of Paramedics, EMTs
To stave off longer 911 call wait times and the closure of ambulance services, many states are rethinking how they recruit and retain both paid and volunteer EMS workers. Nearly 40 state legislatures and Washington, D.C., considered bills in 2022 related to various aspects of emergency medical services, according to the National Conference of State Legislatures.
Damar Hamlin’s cardiac arrest shows need for CPR training and emergency defibrillators in public spaces
Adam Pyle, University of Toronto Football — a sport that involves violent collisions — came under shocking scrutiny on Jan. 2 when Buffalo Bills player Damar Hamlin collapsed from a cardiac event immediately following an on-field collision. Most fans already…
As Overdose Deaths Rise, Few Emergency Rooms Offer Addiction Help
Medical professionals and addiction treatment advocates have long argued that buprenorphine, which is approved by the U.S. Food and Drug Administration, should be available in every emergency room in the country — just like drugs for heart attacks, strokes and diabetic emergencies. And they argue that emergency physicians should have basic training in addiction medicine and be licensed to write a take-home prescription for buprenorphine.
Some Abortion Bans Put Patients, Doctors at Risk in Emergencies
Ever since the U.S. Supreme Court overturned Roe v. Wade, emergency health care providers in states that ban abortion have had to make wrenching legal and ethical judgments before treating a pregnant woman whose health or life may be in peril.
How to stay out of the hospital with omicron here – tips from Public Health – Seattle & King County
How can we keep emergency healthcare from becoming overwhelmed? How can we make sure lifesaving treatment is available when we need it most?
At Urgent Care, He Got 5 Stitches and a Big Surprise: A Plastic Surgeon’s Bill for $1,040
Insurers often try to steer patients to urgent care and away from costly emergency rooms, but individuals could still get hit with large bills in the process.
No Vacancy: How a Shortage of Mental Health Beds Keeps Kids Trapped Inside ERs
If you up in an ER with a mental health crisis, there’s a good chance you will get stuck there.
What Happened When the Only ER Doctor in a Rural Town Got COVID
Papenfus is the lone full-time ER doctor in the town of 900, not far from the Kansas line. ““I’m chief of staff and medical director of everything,” he says.
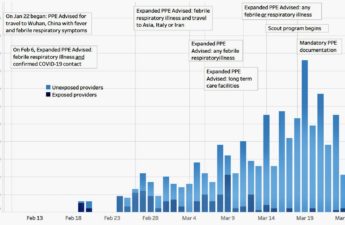
Adjusting tactics quickly cut EMS providers’ COVID-19 risk
These efforts greatly reduced the risk of exposure among EMS providers, reducing the providers’ chance of infection and the number of days they had to be quarantined, and conserving their personal protective equipment (PPE)
‘All the Hospitals Are Full’
On Thursday, 3,812 people were hospitalized with COVID-19 in the region, including more than 1,000 in intensive care units, a record since the pandemic began.
Don’t let COVID-19 keep you from seeking emergency care
Serious symptoms, like those associated with a heart attack or stroke, are still urgent during the COVID-19 pandemic, and rapid treatment is critical.
She Came to New York to Help Fight COVID. She Walked Into a “War Movie.”
My first day in the ER was unlike anything I’d ever witnessed: a mix of a TV show like “Grey’s Anatomy” and something out of a triage tent in a war movie.
“Dead on Arrival”: A N.Y. Fire Chief’s COVID Journal
As New York firefighters respond to coronavirus emergency calls, an FDNY battalion chief and 9/11 survivor confronts the city’s latest mass tragedy.