Category: Immunology
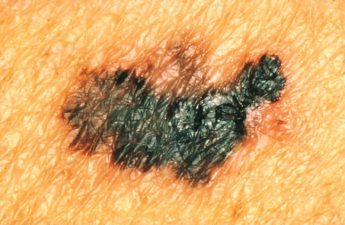
From immunotherapy to mRNA vaccines – the latest science on melanoma treatment explained
Sarah Diepstraten, Walter and Eliza Hall Institute and John (Eddie) La Marca, Walter and Eliza Hall Institute More than 16,000 Australians will be diagnosed with melanoma each year. Most of these will be caught early, and can be cured by…
Nightmares could be an early warning sign of an autoimmune disease flare-up – new study
Many patients could describe nightmares that happened just before their flares. Although patterns varied between different people, they were often similar in each person’s flare-ups. Patients often knew which symptoms were a sign that their disease was about to get worse.
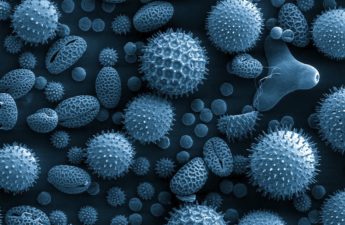
Yes, adults can develop food allergies.
Yes, adults can develop food allergies. Here are 4 types you need to know about
Know Which Medication Is Right for Your Seasonal Allergies
An allergy is your body’s reaction to an otherwise innocent substance that it has identified as an invader. If you have allergies and encounter a trigger (allergen), your immune system fights it by releasing chemicals, such as histamine (hence the term “antihistamine”). Histamine causes symptoms, such as runny nose, itchy nose, sneezing, and itchy and watery eyes.
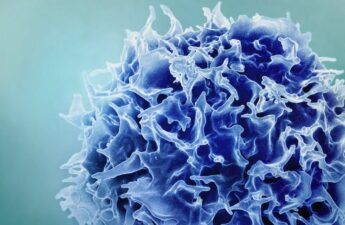
Immune health is all about balance – an immunologist explains why both too strong and too weak an immune response can lead to illness
Many social media posts push supplements and other life hacks that “boost your immune system” to keep you healthy and fend off illness. However, these claims are not based on science and what is known about immune function. Healthy immune systems don’t need to be “boosted.” Instead, the immune system works best when it is perfectly balanced.
Most people who think they are allergic to penicillin aren’t
About 6% of people in the UK are wrongly labelled on their medical records as being allergic to penicillin. This figure is concerning because being labelled as allergic to this class of highly effective antibiotics is associated with an extra six deaths per 1,000 patients a year after being treated for an infection. If patients received the right antibiotic for their infection, many lives could be saved.
Virtual Clinics Embrace Allergy Drops as an Alternative to Shots
An under-the-tongue treatment is popular in Europe, Canada, and Latin America. Why don’t U.S. allergists offer it?
Genetics might explain why some people have never had COVID
. . . but we shouldn’t be too focused on finding out
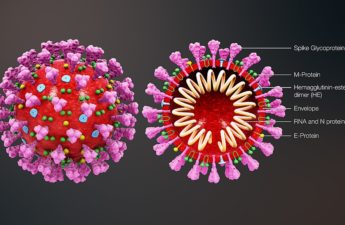
COVID in 2023 and beyond – why virus trends are more difficult to predict three years on
So how will the pandemic be felt in 2023? This question is in some ways impossible to answer, given a number of unknowns. In early 2020 the scientific community was focused on determining key parameters that could be used to make projections as to the severity and extent of the spread of the virus. Now, the complex interplay of COVID variants, vaccination and natural immunity makes that process far more difficult and less predictable.
What is the ‘stiff-person’ syndrome affecting Celine Dion?
Celine Dion’s diagnosis of stiff-person syndrome brought a rare neurological diagnosis into the public eye – two neurologists explain the science behind it
COVID-19, RSV and the flu are straining health care systems – two epidemiologists explain what the ‘triple threat’ means for children
The underlying reasons for the convergence of these viruses and the increase in infections so early in the season are not yet clear. But health experts have some clues about contributing factors and what it could mean for the coming months.
What is inflammation?
Two immunologists explain how the body responds to everything from stings to vaccination and why it sometimes goes wrong
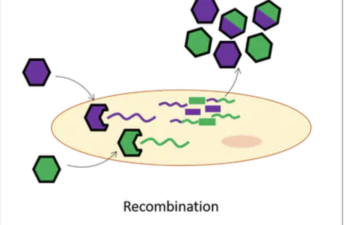
Omicron XE is spreading in the UK – a virologist explains what we know about this hybrid variant
Recombination occurs when two different variants infect the same cell, in the same person, at the same time. From there, they can combine their genetic material, resulting in a virus that possesses a mix of genes from both infecting “parent” viruses. This recombinant variant may then spread to other people – as has been the case with omicron XE.
How does the immune system mobilize in response to a COVID-19 infection or a vaccine? 5 essential reads
We sought out scholars who could take our readers on deep dives into immunology and virology to help demystify these sometimes confusing, conflicting and taxing science-based questions. Here are five stories from The Conversation’s archives that highlight critical insights that we as editors and readers have gained thanks to COVID-19, and that will no doubt continue to be an important part of our pandemic lexicon.
How long does protective immunity against COVID-19 last after infection or vaccination? Two immunologists explain
Upon vaccination or infection with COVID-19, your body produces two types of protective immune responses. The first type involves B cells, which produce antibodies, the second involves T cells, your second line of defense.