Category: Seniors
Medicare Open Enrollment Opens Next Week
Medicare Open Enrollment starts next week! It’s your chance to review or change your prescription drug and health coverage for next year.
Delirium: this common and frightening syndrome looks like dementia, but comes on much faster
Delirium is a common complication of hospitalization can have a direct impact on patients’ illness and mortality rates. It is therefore extremely important to prevent it, or, failing that, to establish an early diagnosis in order to treat it correctly.
How to improve your flexibility – the body’s secret weapon for staying healthy and active
Flexibility might not be the first thing that comes to mind when you think about health and fitness, but it’s one of the most important aspects of maintaining your body’s overall wellbeing.
Accidental falls in the older adult population: What academic research shows
Accidental falls are among the leading causes of injury and death among adults 65 years and older worldwide. As the aging population grows, researchers expect to see an increase in the number of fall injuries and related health spending.
Older adults want to cut back on medication, but study shows need for caution
Many with heart issues or diabetes say they’d like to take less medication, but pharmacists and prescribers need to offer personalized guidance for deprescribing
Looking for nursing home info?
Medicare.gov makes it easy to find and compare nursing homes in your area. Personalize your results by filtering for what matters most to you — like inspection results, location, quality ratings, and more.
Millions of older people don’t get enough nutrients – how to spot it and what to do about it
Weight loss in older adults is a key sign of malnutrition that needs to be addressed – but it can be easily missed, especially when many older adults associate the idea of thinness with good health. But clothing that’s too loose or a watchstrap that floats on the wrist are all warning signs of undernourishment.
More than a third of people with dementia don’t know they have it – what to do if you suspect your partner has the condition
Dementia can present very differently in each person, so it’s about knowing what’s normal for your loved one. A person who has always been conscientious and organised starting to unravel is very different from a scatterbrained person just being slightly more scatterbrained.
Older adults want to ‘age in place,’ but their options are limited in most states
As America gets grayer, advocates are pushing for new types of housing. By Robbie Sequiera, Staff ReporterStateline As older adults begin to outnumber young people in the United States in the coming decade, advocacy groups are challenging states to shift…
Early indicators of dementia: 5 behaviour changes to look for after age 50
Five signs to look for: Apathy, affective dysregulation, lack of impulse control, social inappropriateness, and abnormal perceptions or thought.
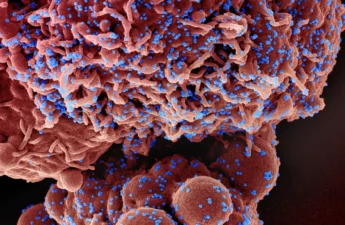
COVID-19 vaccine boosters are the best defence: Older adults shouldn’t rely on previous infection for immunity
We found that those who had battled the BA.1-2 variant of Omicron in early 2022 had a 30-fold higher risk of contracting the BA.5 variant later in the year. That was exactly the opposite of what we, or anyone, would have predicted. What the findings do tell us is that older adults who have had a previous COVID-19 infection shouldn’t rely on that to protect them against reinfection this fall. To protect against severe illness, keeping booster shots up to date is recommended.
Biden Administration Proposes New Standards to Boost Nursing Home Staffing
The nation’s most thinly staffed nursing homes would be required to hire more workers under new rules proposed on Friday by the Biden administration, the greatest change to federal nursing home regulations.
There’s no age limit for politicians − as people live longer, should that change?
Joe Biden, Mitch McConnell and Diane Feinstein are all over 80 years old, joining a number of politicians who are staying in office well past their 70s.
Am I too old to build muscle?
What science says about sarcopenia and building strength later in life
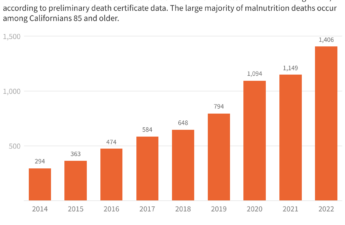
The number of elderly dying of malnutrition in the US has more than doubled since 2018
In California the rate of elderly dying of malnutrition has accelerated, Phillip Reese reports.